Phone: 0141 943 3300
72 Drymen Road, Bearsden, Glasgow G61 2RH
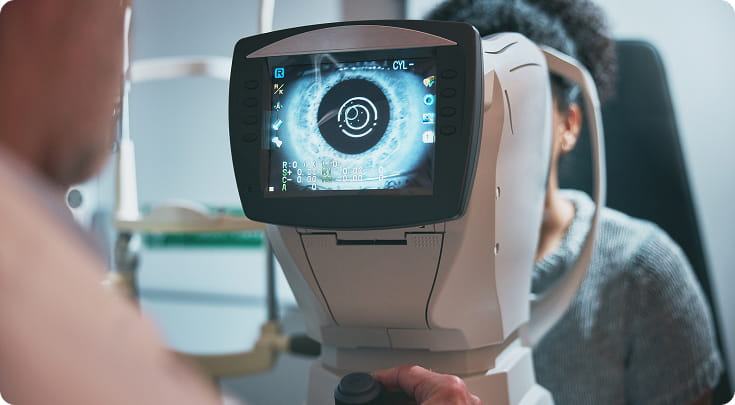

If you’ve been living with dry, gritty, burning, watery or light‑sensitive eyes for months (or years)… and you’ve already tried drops, gels, warm compresses, lid wipes — maybe even seen multiple opticians, your GP, or ophthalmology — you’re exactly who our clinic is designed for.
At Peter Ivins Eye Care (Bearsden, Glasgow), our specialist dry eye clinic uses state‑of‑the‑art imaging and in‑house tear testing to identify why your eyes are uncomfortable — then builds a personalised plan to improve comfort and stability long‑term.

Initial assessment typically takes 60–90 minutes, allowing a full history, imaging, testing, and a clear treatment plan.

We measure tear stability, tear volume, lipid layer quality, blink behaviour, and meibomian gland health — then track change over time.

We produce a detailed dry eye report and treatment plan so you understand what’s going on and what we’re doing about it.
Peter Ivins Eye Care was established in 2010 with a stated commitment to combining high standards of clinical care with advanced diagnostic equipment and ongoing reinvestment in technology.
The practice was the first in Scotland introduce the Oculus K5 imaging, meibography and diagnostic suite in 2014; to offer BlephEx treatment of blepharitis in 2014, Scleral contact lens fitting for dry eye in 2015; IPL treatment of MGD in 2016; meibomian gland probing in 2017 and amniotic membranes for dry eye in 2019.


You may benefit if you have:
Below is the structure of our assessment and why each step matters.
We start with a deep dive into:
We measure how quickly your tears become unstable between blinks — a core indicator of evaporative dry eye.
We assess tear quantity without touching the eye where possible, including tear meniscus evaluation.
The lipid (oil) layer reduces evaporation. We image and grade lipid layer quality and thickness to understand whether the tear film is evaporating too fast.
We assess how the tear film behaves over time (including movement/ viscosity patterns) which supports accurate diagnosis and monitoring.
We map corneal shape and surface integrity — important in ocular surface disease, contact lens complications, and irregularity that can worsen symptoms.
We document surface redness patterns objectively, giving us a baseline we can track as treatment begins.
Blink quality and completeness matter — especially with screen use and modern lifestyle. We assess blink patterns and their impact on tear stability.
If non‑invasive measures suggest aqueous deficiency, we may use traditional tests to quantify tear volume more directly
InflammaDry helps measure inflammatory markers in the tear film so we can decide whether inflammation‑targeted treatment should be part of your plan.
We use clinical dyes to assess the health of the ocular surface and identify staining patterns — key for grading severity and tailoring treatment.
You leave with:
Most initial assessments take 60–90 minutes, allowing time for a full history, imaging, tear testing, and a personalised plan.
No — the majority are non-invasive. Some drops may sting briefly, but the clinic approach is designed to be comfortable while still gathering the data needed to tailor treatment.
Drops can temporarily soothe symptoms, but many cases require identifying and treating the underlying drivers (e.g., tear evaporation, lid inflammation, meibomian gland dysfunction, inflammation markers).
You can make an appointment with our expert.
You can also use our online appointment system.
| Monday | |
| Tuesday | |
| Wednesday | |
| Thursday | |
| Friday | |
| Saturday | |
| Sunday | Closed |